When a breakthrough innovation, new test, or new treatment is discovered in medicine, its adoption often follows a typical pattern. This pattern is demonstrated graphically on the illustration below. I have adapted this concept from the Hype Cycle used to describe new technologies in business but with some important modifications.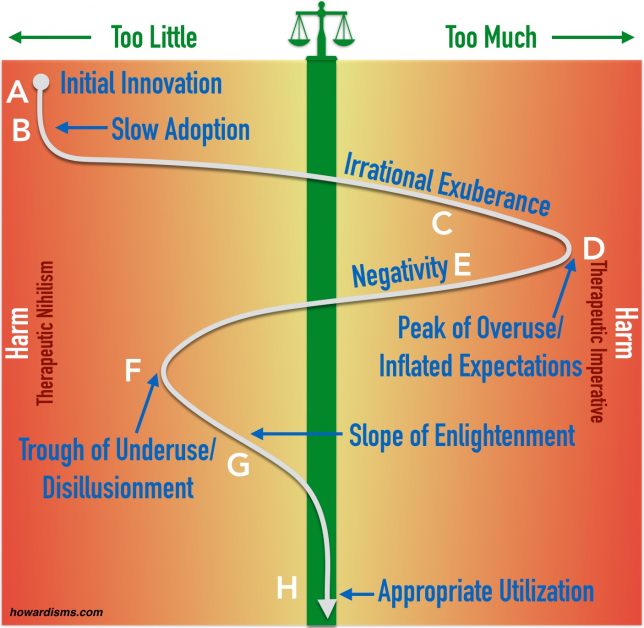
A new discovery is made at Point A. For a time there is slow adoption (A to B). During this time, patients are being harmed because they are not benefiting from the new discovery due to a lack of access. This period can last anywhere from months to decades and is dependent on several factors:
- How revolutionary is the idea? How much does it unsettle the status quo?
- Insulin and antibiotics made it from lab bench to market incredibly fast because the benefit was so obvious and so dramatic. Geocentrism lingered for nearly a century after it should have been abandoned because it too much upset the status quo.
- Who is promoting the idea? Does someone stand to make a lot of money before a patent expires?
- Pharmaceutical companies and device makers are highly skilled at extracting every cent out of a new product before the patent expires; they do this by promoting indication drift for their products among physicians who are too impressionable.
Eventually, the new idea takes off and the innovation is not only applied to the indication for which it was discovered, but also to things similar to that indication. This period of irrational exuberance (C) is filled with diagnostic and indication drift, and the innovation is heralded as the answer to everything, the great breakthrough that will change the whole world. Just how irrational this exuberance becomes is affected by several things:
- How beneficial was the initial breakthrough? How much of a miracle (think insulin or penicillin), how big a breakthrough (think DNA)?
- How much money is being made and by how many different sectors? Does just the pharmaceutical company stand to make a profit or do hospitals and doctors stand to gain as well? Gain is not just financial, but professional as well since many careers are made or broken on some new “breakthrough.”
By the peak of overuse at Point D, there is usually some growing discontent. Payers are tired of being exploited by paying for an innovation that doesn’t seem to be worth it; long-term and reproduced studies are increasingly showing a lack of benefit, particularly for the now greatly-expanded indications. Harms are starting to be seen as long-term results stream in, especially in patients who are not benefiting that much. The literature is mature enough to call almost any perceived benefit into question.
Now, negativity sets in (E) and usage declines. But this correction is often excessive, as people become increasingly disillusioned with the innovation. There may be lawsuits. The media may over-exaggerate the harms and underestimate the benefits. Alternative health practitioners will seek to use the innovation as an example of why science-based medicine cannot be trusted. Pharmaceutical companies may have a new patented drug to promote and so paint the old drug in the worst possible light. This emotional reflex leads to underuse of the innovation.
(Think about artificial sweeteners: Cyclamate gave way to Saccharin, Saccharin gave way to Aspartame, Aspartame gave way to Sucralose, now Sucralose is being pushed out for Stevia or some other alternative. Why? Competition. None of the agents ever caused cancer or weight gain or autism or anything else. But when there is new money to be made, suddenly safety claims are made about the current market leader to scare the public to some alternative. Same thing with pharmaceuticals. Statins are currently being pushed out for PCSK9 inhibitors not by science, but by marketing).
There are generational influences on this cycle, as well. As every generation tends to think of itself as smarter than the last (“We have arrived! Our parents were clueless buffoons!”), there is a tendency to reject practices of the last generation. Thus, a not so good intervention may be overly-adopted (rejecting the previous generation’s reluctance) and then a decent intervention may be overly-abandoned (rejecting the previous generation’s over-utilization).
Eventually, the emotions die down and the evidence matures. This is the Slope of Enlightenment (G) where a more rational and evidence-based rationale develops for utilization of the innovation, hopefully leading to Point H, or appropriate utilization.
This entire cycle can take years to decades and it can actually repeat itself.
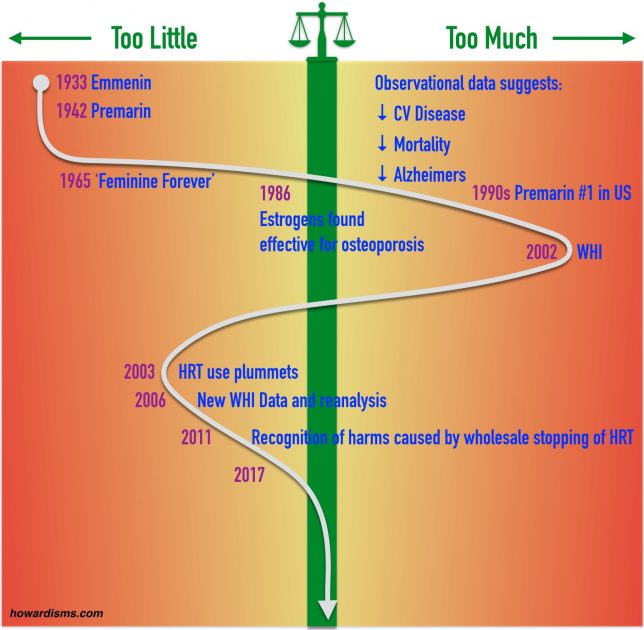
Let’s look at an example of an innovation on the Cycle: female hormone replacement.
In 1933, Emmenin, a conjugated estrogen product, was released to the market. It was extracted from the urine of pregnant women and was therefore very expensive to manufacture with limited production abilities. This limited the promotion and availability of the drug, and therefore it’s early adoption. DES was released in 1939, and they sold every pill they could manufacture. In 1941, Ayerst Laboratories began marketing Premarin, which was a conjugated estrogren made from the urine of pregnant mares. It was marketed to treat hot flashes and other menopausal symptoms and sales began to take off. Soon, Premarin became the dominant estrogen on the market.
At this point, there were no efficacy studies for Premarin or other estrogens and the quality of safety studies was about as good as the quality of safety studies performed for DES (which both didn’t work and went on to harms thousands of women). But women with menopausal symptoms who took Premarin did feel better and intense marketing convinced women (and their husbands) to demand the medicine from physicians who might otherwise have been a little skeptical about it.


Those advertisements are worth reading. In 1965, a book by Dr. Robert Wilson entitled Feminine Forever made wild claims about the ability of Premarin to change women’s lives. It was the great panacea that fixed every problem an older woman might have. The cover claimed,
A fully documented discussion of one of medicine’s most revolutionary breakthroughs – the discovery that menopause is a hormone deficiency disease, curable and totally preventable, and that every woman, no matter what her age, can safely live a fully-sexed life for her entire life.
Wilson claimed in the book that it had been proven that estrogen didn’t cause cancer, but rather prevented it, and that menopausal women were unnaturally and prematurely castrated – that menopause was an unnatural, diseased state. Premarin was the fountain of youth and the key to longevity. This book spurred real growth in Premarin sales and encouraged many false beliefs about its efficacy among physicians and patients alike. What was not mentioned in the book was that the research behind the book and the best-selling book itself were paid for by Wyeth, the maker of Premarin. It was simply a marketing tool.
Still, the world understood estrogen differently after this book was published, and even though the FDA sanctioned Wilson in 1969, women everywhere thought Premarin was the key to immortality. In 1986, Premarin and other estrogens were found to be protective against osteoporosis. This was, perhaps, the first real science surrounding the efficacy of estrogens and it was used by the true believers as evidence that all the previous claims about Premarin were true. Soon, low quality observational data was being published that indicated that Premarin lowered the risk of cardiovascular disease, lowered the risk of Alzheimer’s disease, and led to decreased mortality for the women who took it. This was the sam type of data that indicates a link between autisms and vaccines, but it was eagerly seized upon by those who had money to make.
In the meantime, a definitive connection had been made between unopposed Premarin and uterine cancer, but this was fixed with the introduction of Prempro which added progesterone into the mix. By the late 1990s, Premarin was the top selling drug in the US and a woman was lucky to make it past the age of 51 without a prescription for either Premarin or Prempro. This was the peak of overuse and inflated expectations. It was not based on science but rather fueled by indication drift and clever marketing.
Then the Women’s Health Initiative (WHI) happened. This large trial was designed to determine if the non-evidence based claim that HRT reduced the risk of cardiovascular disease was true. The study was stopped prematurely in 2002 after preliminary data indicated that Premarin and Prempro might actually increase the risk of heart disease and breast cancer, not to mention blood clots.
The negativity was immediate and came from all corners. Some curmudgeon doctors, who for years had quietly been suggesting that HRT increased the risk of breast cancer, gloated and wrote books and sermonized. Oprah Winfrey and other media figures told women that they had been lied to and deceived by the medical establishment. Women felt betrayed by their doctors. Alternative medicine practitioners crucified “Big Pharma” and discovered every unethical marketing ploy Wyeth had ever used to market the drug. Propaganda was disseminated and exaggerated by those who sought to make a buck off the situation, in the form of “bioidentical hormones.” The FDA reacted in a knee-jerk manner. Oncologists vilified estrogen as the cause of breast cancer. Women stopped their hormones by the millions almost overnight.
But, of course, the reality is that HRT was neither an abysmal, evil villain murderously ravaging women nor the fountain of youth that had been promised to save them all. It helped some women, improved their quality of life, and also hurt some women. We are somewhere, now, on the slope of enlightenment, realizing that it was neither as good as the people selling it would have us believe and nowhere near as bad as those selling something on the other extreme would have us believe. Today, HRT is being underutilized, but the literature is maturing and we are more able to accurately state its risks and benefits than ever before.
We realize today that thousands of women were harmed when the use of HRT was abandoned; many thousands likely died premature deaths. Estrogen wasn’t associated with an increased risk of breast cancer after all, but progesterone might be. It’s complicated. Really, really complicated. One size doesn’t fit all, and things are not all good or all bad. That’s the difficult thing about “science:” it doesn’t prove or disprove anything, and even though a study might only deal with a single outcome, the intervention affects many things simultaneously. Unintended consequences abound. Birth control pills might increase the risk of breast cancer (doubtful) but they concurrently decrease the risk of ovarian cancer by a much greater magnitude. We have to take the good with the bad.
The sad thing is, this cycle for HRT and most other innovations is completely avoidable (read this, please). But to avoid these wild swings, physicians must learn to weight evidence appropriately instead of emotionally bounding from one extreme to the other.
Let’s look at where some other things are on the Herrell Curve (or whatever you want to call it):
I won’t go through each of these here in detail. I’ll let you think about it. Let me know if you disagree. I will point out that the only thing on the list that is probably appropriately utilized is Anti-D Antibody, though even that is slightly overused (which is okay). It’s interesting to think about why anti-D antibody is the most appropriately utilized intervention: because the indication is very clear. It is to be used for women with Rh negative blood. The circumstances requiring its use are a little wandering, though. Do Rh negative women with a 5 week miscarriage need it? Probably not. But overall, it is fairly clear-cut who should receive it and its easy to teach a medical student. Where there is clarity, there is no decision. Why can’t other things be this simple?
The problems start when drift or polarized thinking occurs. If a robotic hysterectomy is good for an ovarian cancer staging case, maybe it’s good for a benign hysterectomy, too? No. If a biophysical profile is good for a woman with medication controlled diabetes, maybe it’s also good for a woman with diet-controlled diabetes? No. Is Vitamin D the miracle nutrient that single-handedly cures and prevents all disease? No. Are mechanical morcellators death-wielding, cancer-causing agents of destruction? No.
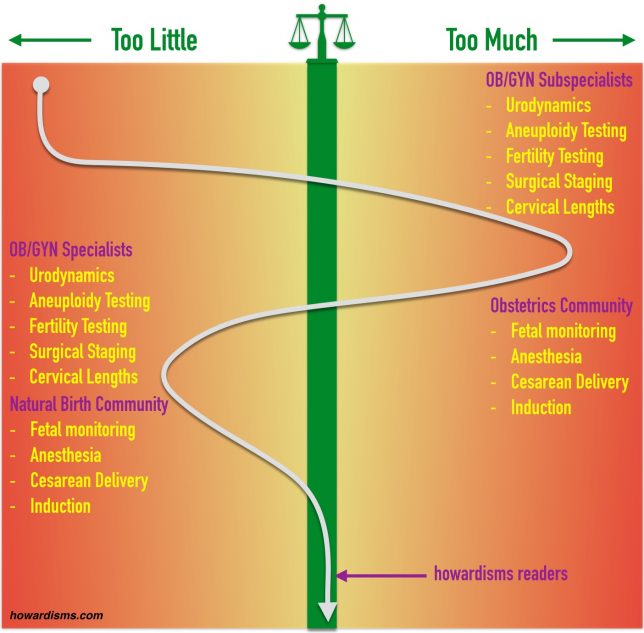
Of course, not everyone is at the same place on the Herrell Curve. It depends on what your interests and motivations are. For example, take a look at this one:
Subspecialists in Ob/Gyn grossly over-utilize their common interventions, believing them more beneficial or more effective than they actually are and profiting along the way. The general obstetrics community also over-utilizes its common interventions for the same reasons. Meanwhile, Ob/Gyn specialists often under-appreciate the value of some interventions while the natural birth community polarizes all the interventions and declares them all bad, all the time. The truth is usually in the middle.
What can you do?
- Be aware of the cycle and recognize where things are on it.
- Look for actual evidence of actual outcomes that matter before jumping on board with the latest fad.
- Don’t over-estimate the magnitude of effect of a particular intervention and don’t be too dogmatic about it.
- Change as new evidence develops.
- Appreciate that things aren’t all good or all bad. All things are potentially both good and bad and all things need to be delivered in the right dose for the right condition. Don’t think in polarized terms. Define the good and define the bad for everything you do and own it.
- Interpret evidence critically.
- Know the evidence for what you believe and how you practice.
- Use Bayesian inference when making decisions about medical interventions. If you don’t know what that means or how to do it, learn.